A new publication in The Lancet HIV highlights the lack of research on key populations of women most likely to experience intimate partner violence and HIV, and recommends strategies to address.
Globally, women from marginalized communities – those who use drugs, engage in sex work, are transgender, or are adolescents and experience intimate partner violence – have been missing from surveillance research (research that captures the prevalence and incidence on types of violence) and prevention and treatment strategies and policies. Though significant efforts have been made to include them, because these populations are so marginalized, representative data on the rates of intimate partner violence (and sometimes HIV) are difficult to obtain.
A new publication addresses this gap.
Read the publication: Intertwined epidemics: progress, gaps, and opportunities to address intimate partner violence and HIV among key populations of women (pdf)
Most mainstream intimate partner violence prevention efforts have focused on general populations of women, not on the aforementioned key populations of women, despite their risks for experiencing intimate partner violence being much higher.
In fact, DrPH candidate and second author Trena Mukherjee shares "I think one of the most important findings is the complete lack of intimate partner and HIV interventions that address unique risk factors for transgender populations, despite them having some of the highest rates of both intimate partner violence and HIV."
Similar to addressing HIV, focusing on the general population misses the mark and ignores the broader social forces and social determinants of health that drive the intertwined epidemics of intimate partner violence and HIV among women in marginalized communities. Integrated approaches that address both simultaneously are more likely to be effective at reducing risk factors that contribute to intimate partner violence and HIV transmission, improve related health outcomes, and provide cost savings.
[There are a] complete lack of intimate partner and HIV interventions that address unique risk factors for transgender populations, despite them having some of the highest rates of both.
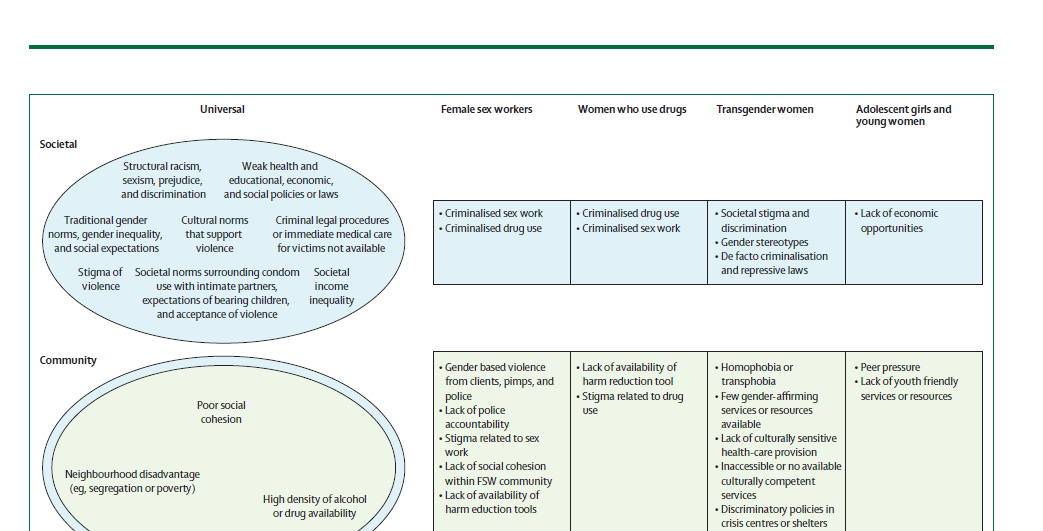
In the Figure linked and excerpted below, the authors share risk factors for intimate partner violence for specific key populations of women including female sex workers, transgender women, women who use drugs, and adolescent girls and young women.
Over the past two decades, numerous multi-level IPV interventions have been developed and shown to be effective in reducing IPV and HIV among different populations of women from marginalized communities around the world. However, to date, the vast majority of these interventions have not been used or scaled up due to lack of resources and funding. The authors share:
“Additionally, little attention has been paid to economic evaluations that could support scaling-up and integration of combination IPV/HIV interventions into routine practice and policy.”
There also remains a critical need for implementation research to inform optimal strategies for delivering these interventions in resource constrained settings that serve women from marginalized communities.
Project WINGS Reduces Violence Against Women in India
The authors of the paper underscore the need for tailored interventions, prevention and policy approaches, to include a network of providers working together:
“The intertwined epidemics of intimate partner violence and HIV must be addressed among key populations, to achieve the UNAIDS 95–95–95 targets. This requires greater investment to support research that includes intimate partner violence surveillance and evaluates the efficacy, implementation, and cost-effectiveness of novel combination interventions tailored for key populations of women, as well as funding for community based organisations to implement evidence-based interventions for key populations in real-world settings.”
First-author Dr. Nabila El-Bassel, who 30 years ago founded the Social Intervention Group to address the AIDS pandemic, states that “Few research and prevention efforts or policies focus on intimate partner violence and HIV among key populations of women, despite these women bearing a disproportionate burden of both. Globally the emphasis needs to be on changing policy. Intimate partner violence needs to be part of the equation to end HIV.”
A combination HIV risk reduction and microfinance intervention for female sex workers who use drugs in Kazakhstan
Key populations of women need combination intimate partner and HIV interventions
This publication advocates for greater attention from researchers, governments, and policymakers to incredibly high rates of intimate partner violence among the most vulnerable groups of women, and the need to reduce both partner violence and HIV incidence and improve access to the HIV care continuum.
There is an urgent need for combination intimate partner violence and HIV interventions for transgender populations. The authors did not identify any such interventions, despite an extremely high risk of both intimate partner violence and HIV.
This publication invites scientists, researchers, funders, health equity leaders, and policymakers interested in the well-being of women, and ending HIV and violence against women, to read these findings carefully.
Few research and prevention efforts or policies focus on intimate partner violence and HIV among key populations of women, despite these women bearing a disproportionate burden of both. Globally the emphasis needs to be on changing policy. Intimate partner violence needs to be part of the equation to end HIV.
The publication, “Intertwined Epidemics: Progress, gaps, and opportunities to address intimate partner violence and HIV among key populations of women,” was authored by
- Dr. Nabila El-Bassel, University Professor at Columbia and Director of the Social Intervention Group;
- Trena I Mukherjee, MPH, Department of Epidemiology, Mailman School of Public Health, Columbia University;
- Claudia Stoicescu, PhD, School of Social Work, Columbia University and Centre for Criminology, Centre for Evidence-Based Social Intervention, University of Oxford;
- Laura E Starbird, PhD, School of Nursing, University of Pennsylvania;
- Jamila K Stockman, PhD, Division of Infectious Diseases and Global Public Health, Department of Medicine, University of California San Diego;
- Prof Victoria Frye, PhD, School of Medicine, The City University of New York;
- Prof Louisa Gilbert, PhD, School of Social Work, Columbia University.